Stem Cell Essentials
Mesenchymal Stem Cells (MSCs)
MSCs are self-renewing, multipotent precursors to other cell types and tissues. Scientists have found MSCs in many tissues from young to old. As we age, we appear to have fewer MSCs with the older MSCs typically behaving differently from the younger MSCs. MSCs have exciting potential and have shown great promise, whether we use our own aged MSCs or a graft from postnatal sources.
MSCs have demonstrated indirect local effects (similar to paracrine activity) that appears to be active for many weeks – possibly longer. It is thought that they may be responding to their local environment and, like healthy refreshed soldiers, may be able to effect change and regeneration in a customized way the host cells may no longer be fully capable of.
Postnatal tissues have high concentrations of MSCs across multiple compartments/tissues and these MSCs exhibit a more robust secretome and more rapid cell division frequency yet with a lower rate of teratogenesis.
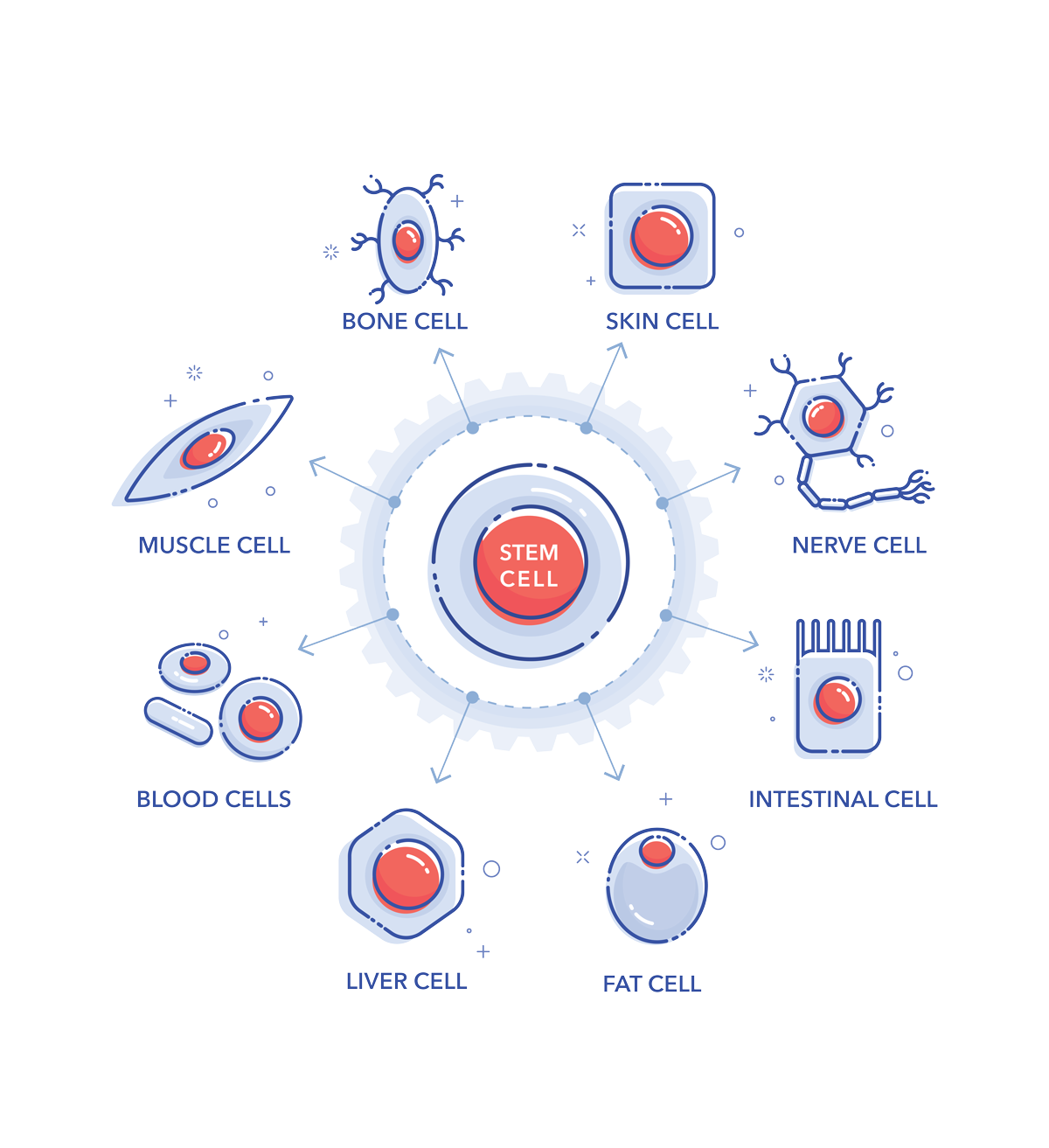
Types of Stem Cells

Totipotent Stem Cells
Also known as embryonic stem cells, totipotent cells can become extraembryonic (placental cells/tissue). “Totipotent” means that these cells can differentiate into any type of cell or tissue which would indicate vast potential. However, because of the risks of teratoma, this type of stem cell is unsuitable for therapeutics and using it is illegal in the United States.

Pluripotent Stem Cells
Pluripotent stem cells can differentiate into any of the cell types in a body. Pluripotent cells give rise to the endoderm, mesoderm, and ectoderm.

Multipotent Stem Cells
These cells give rise to many types of cells but are more limited than pluripotent cells. Multipotent stem cells are found in postnatal umbilical cord and placenta tissues, as well as in adult tissues. They serve as a reservoir of cells for growth and repair. Each type of multipotent stem cell gives rise to a limited range of cell types. These cells are more difficult to isolate for clinical use but are ethical. Examples of multipotent stem cells include hematopoietic stem cells (HSC) and mesenchymal stem cells (MSC).
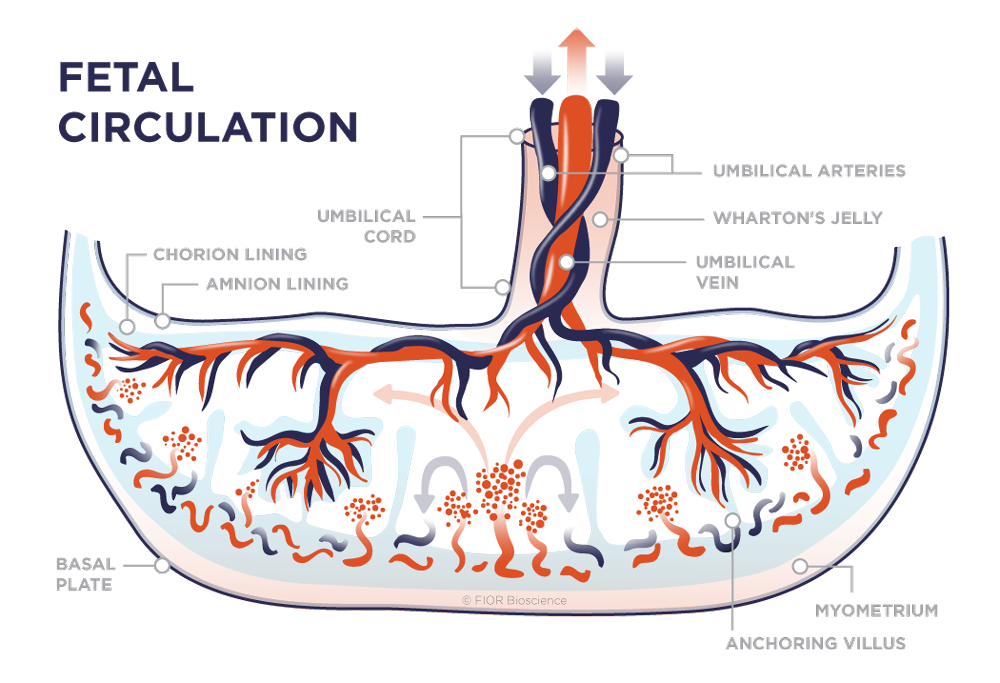
MSC's in Postnatal Tissues
MSC’s were first identified in the adherent fraction of bone marrow stroma. They were termed CFU-Fs because of their ability to generate single cell-derived colonies, in analogy to their hematopoietic counterparts, CFU-Fs from almost all embryonic and postnatal tissues can be expanded in vitro to generate cell cultures that conserve trilineage potential. The role of MSC’s in multiple anatomical locations, and whether they constitute a specific homogeneous cell type or a mixed population of tissue-specific cells heterogenous in nature and origin, is not well understood. However, these progenitors express pericyte-specific cell-surfaced markers such as NG2 and PDGRRB and are located in perivascular regions of the different tissues in which they reside.

MSC Expansion in Vitro
MSC’s can be expanded in vitro when cultured in two-dimensional monolayers of adherent cells in specialized medium. The expanded cells sometimes termed multipotent mesenchymal stromal cells are defined by the expression of CD73, CD90 and DC105 and the lack of CD11b, CD19, CD34, CD45 and HLADR. Here we use the term mesenchymal stromal cells to refer to these in vitro-expanded cells.
MSC Differentiation Potential
The principal criterion defining multipotent mesenchymal stromal cells is their ability to differentiate into mature adipocytes, chondrocytes and osteoblasts when placed in specific culture conditions.